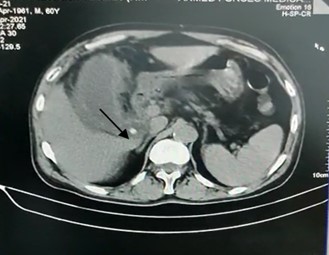
A case of acute calculous cholecystitis with contained gall bladder perforation with pericholecystic collections extending to liver parenchyma
Abstract
Gall bladder perforation is a serious complication of acute cholecystitis and represents an advanced stage of the disease. Its clinical presentation is varied and can range from non-specific symptoms to acute generalized peritonitis. In many cases, GB perforation in diagnosis during exploratory laparotomy for peritonitis and with no definite source identified. The presentation of gall bladder perforation can be indistinguishable from uncomplicated acute cholecystitis. A 60 yrs. old male with no known comorbidities presented to a tertiary care hospital with diffuse pain abdomen associated with vomiting and constipation of 04 days’ duration. Clinical evaluation revealed icterus and tenderness in right hypochondrium and generalized peritonitis. Lab investigations revealed conjugated type hyperbilirubinemia and elevated serum Lipase levels and normal Amylase levels. Initial USG revealed Acute acalculous cholecystitis with normal IHBR and normal CBD. Later NCCT abdomen and MRCP were done which revealed calculous cholecystitis with sealed off GB perforation IHBR, CBD, and normal pancreas. The patient was managed non-operatively and responded well. The inflammatory reaction of the peritoneum in bile peritonitis increases the absorption of the spilled conjugated bile from the peritoneal cavity. The conjugated type hyperbilirubinemia without dilatation of the bile duct on imaging examination was the sign of bile leakage into the peritoneal cavity.
Downloads
References
H. Sethi and C. D. Johnson, “Gallstones,” in Medicine, Elsevier, Philadelphia, PA, USA, 2011.
B. Kessel, A. R. Zeina, I. Ashkenazi, and R. Alfici, “Perforation of the gallbladder into the abdominal wall: a rare manifestation of biliary disease,” Radiology Case Reports, vol. 9, no. 1, p. 866, 2015.
S. Sen and U. K. Parui, “Spontaneous gall bladder perforation: a rare clinical entity, a diagnostic and surgical challenge,” Surgical Medicine Open Access Journal, vol. 1, no. 1, pp. 1–4, 2018.
B. P. Reines and B. W. Ninham, “Structure and function of the endothelial surface layer: unraveling the nanoarchitecture of biological surfaces,” Quarterly Reviews of Biophysics, vol. 52, p. e13, 2019.
T. N. Van Diepen, S. Van Esch, D. G. Struijk, and R. T. Krediet, “The first peritonitis episode alters the natural course of peritoneal membrane characteristics in peritoneal dialysis patients,” Peritoneal Dialysis International: Journal of the International Society for Peritoneal Dialysis, vol. 35, no. 3, pp. 324–332, 2015.
H. Derici, E. Kamer, C. Kara, et al., “Gallbladder perforation: clinical presentation, predisposing factors, and surgical outcome of 46 patients,” The Turkish Journal of Gastroenterology, vol. 22, no. 5, pp. 505–512, 2011.
S. A. Khan, Gulfam, A. W. Anwer, Z. Arshad, K. Hameed, and M. Shoaib, “Gallbladder perforation: a rare complication of acute cholecystitis,” JPMA. The Journal of the Pakistan Medical Association, vol. 60, no. 3, pp. 228-229, 2010.
H. Derici, C. Kara, A. D. Bozdag, O. Nazli, T. Tansug, and E. Akca, “Diagnosis and treatment of gallbladder perforation,” World Journal of Gastroenterology, vol. 12, no. 48, pp. 7832– 7836, 2006.
H. Chowdhury and D. N. Lobo, “Gallstones,” in Surgery- Elsevier, Philadelphia, PA, USA, 2011.
D. Q. Wang and N. H. Afdhal, Gallstone Disease in Sleisenger and Fordtran’s Gastrointestinal and Liver Disease: Pathophysiology, Diagnosis, and Management, Elsevier, Phila- delphia, PA, USA, 2015
S. L. Gans, J. Stoker, and M. A. Boermeester, “Review-plain abdominal radiography in acute abdominal pain: past, present, and future,” International Journal of General Medicine, vol. 5, pp. 525–533, 2012.
R. D. Brown, I. Zanzi, G. Harris, and R. Alhindawi, “Gall-bladder perforation and hepatobiliary scintigraphy,” Clinical Nuclear Medicine, vol. 29, no. 10, pp. 644-645, 2004.
M. K. Dutt, G. M. Murphy, and R. P. Thompson, “Unconjugated bilirubin in human bile: the nucleating factor in cholesterol cholelithiasis?” Journal of Clinical Pathology, vol. 56, no. 8, pp. 596–598, 2003.
P. Mukerjee, J. D. Ostrow, and C. Tiribelli, “Low solubility of unconjugated bilirubin in dimethylsulfoxide water systems: implications for pKa determinations,” BMC Biochemistry, vol. 3, no. 1, p. 17, 2002.
Bulmer, J. Coombes, J. Blanchfield, I. Toth, R. Fassett, and S. Taylor, “Bile pigment pharmacokinetics and absorption in the rat: therapeutic potential for enteral administration,” British Journal of Pharmacology, vol. 164, no. 7, pp. 1857– 1870, 2011.
B. J. Barber, T. J. Schultz, and D. L. Randlett, “Comparative analysis of protein content in rat mesenteric tissue, peritoneal fluid, and plasma,” American Journal of Physiology-Gastro- intestinal and Liver Physiology, vol. 258, no. 5, pp. G714–G718, 1990.
T. Kamisako, Y. Kobayashi, K. Takeuchi, et al., “Recent advances in bilirubin metabolism research: the molecular mechanism of hepatocyte bilirubin transport and its clinical relevance,” Journal of Gastroenterology, vol. 35, no. 9, pp. 659–664, 2000.
M. Amberger, N. Burton, G. Tissera, G. Baltazar, and S. Palmer, “Spontaneous common bile duct perforation-a rare clinical entity,” International Journal of Surgery Case Reports, vol. 46, pp. 34–37, 2018.
P. Chaudhary, A. Kumar, N. Saxena, and U. C. Biswal, “Hyperbilirubinemia as a predictor of gangrenous/perforated appendicitis: a prospective study,” Annals of Gastroenterology, vol. 26, no. 4, pp. 325–331, 2013.
Y. R. Hong, C.-W. Chung, J. W. Kim, et al., “Hyperbilirubinemia is a significant indicator for the severity of acute appendicitis,” Journal of the Korean Society of Coloproctology, vol. 28, no. 5, pp. 247–252, 2012.
T. Nishida, N. Fujita, T. Megawa, M. Nakahara, and K. Nakao, “Postoperative hyperbilirubinemia after surgery for gastro-intestinal perforation,” Surgery Today, vol. 32, no. 8, pp. 679–684, 2002.
C. M. Lee, L. Stewart, and L. W. Way, “Postcholecystectomy abdominal bile collections,” Archives of Surgery, vol. 135, no. 5, pp. 538–544, 2000.
Niemeier OW. Acute Free Perforation of the Gall-Bladder. Ann Surg. 1934 Jun;99(6):922–924
Jethwani U, Singh G, Mohil RS, Saroha R, Chouhan J, Bansal N. Gall bladder perforation: report of two cases. OA Case Reports 2013 Jul 12;2(5):50.