Sociodemographic status of hemorrhagic stroke patients: A study in a tertiary care hospital of Bangladesh
Abstract
Background: Worldwide, stroke is the second cause of death and the third cause of disability. For the prevention of hemorrhagic stroke as well as for reducing stroke-related mortality and disability knowledge of the sociodemographic status of hemorrhagic stroke patients is very important.
Aim of the study: The aim of this current study was to assess the sociodemographic status of patients with hemorrhagic stroke.
Materials and Methods: This observational cross-sectional study was carried out at Neurology and Medicine ward Mymensingh Medical College Hospital (MMCH) from July 2017 to December 2018. In total 60 subjects of more than 18 years were considered for the study as the study subjects. The study population had been selected according to the pre-defined exclusion and inclusion criteria. Only patients with hemorrhagic stroke attended the mentioned hospital ware included. All data were processed, analyzed, and disseminated by MS Office and SPSS programs as per need.
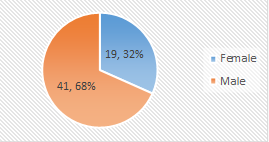
Results: In this study, among a total of 60 participants, 68% (n=41) were male whereas the rest 32% (n=19) were female. The majority of the patients were from 50 years and above age groups which were 63.33% of the total respondent. One-third (33%) of the total study population were service holders which was the highest number from a single profession. The majority of the patients were from lower middle-classed families which were 63.33%. The highest number of participants were from peri-urban areas which were 43%. As the risk factors, smoking, DM as well as HTN were found among 65%, 12%, and 77% of patients respectively.
Conclusion: The ratio of male hemorrhagic stroke patients is higher. Although living area, economic status, and residence area may not be correlated with hemorrhagic stroke, age, the habit of smoking and HTN may arise as some potential risk factors for hemorrhagic stroke.
Downloads
References
Johnson, W., Onuma, O., Owolabi, M., & Sachdev, S. (2016). Stroke: a global response is needed. Bulletin of the World Health Organization, 94(9), 634.
Allen, L. N., Pullar, J., Wickramasinghe, K. K., Williams, J., Roberts, N., Mikkelsen, B., & Townsend, N. (2018). Evaluation of research on interventions aligned to WHO ‘Best Buys’ for NCDs in low-income and lower-middle-income countries: a systematic review from 1990 to 2015. BMJ global health, 3(1), e000535.
Feigin, V. L., Forouzanfar, M. H., Krishnamurthi, R., Mensah, G. A., Connor, M., Bennett, D. A., & Murray, C. (2010). Global Burden of Diseases. Injuries, and Risk Factors Study, 1990-2010.
O'donnell, M. J., Xavier, D., Liu, L., Zhang, H., Chin, S. L., Rao-Melacini, P., & Yusuf, S. (2010). Risk factors for ischaemic and intracerebral haemorrhagic stroke in 22 countries (the Interstroke study): a case-control study. The Lancet, 376(9735), 112-123.
Khealani, B. A., &Wasay, M. (2008). The burden of stroke in Pakistan. International Journal of Stroke, 3(4), 293-296.
Hu HH, Sheng WY, Chu FL, Lan CF, Chiang BN. Incidence of stroke in Taiwan. Stroke. 1992;23(9):1237-41.
Mohammad, Q. D., Habib, M., Hoque, A., Alam, B., Haque, B., Hossain, S., ... & Khan, S. U. (2011). Prevalence of stroke above forty years. Mymensingh medical journal: MMJ, 20(4), 640-644.
Kibria, M. A., Hassanuzzaman, M., Kayasthagir, P. K., Karim, M. R., Rahman, A., Obaida, A. S. M. A., ... & Faruk, M. G. (2018). Is low total cholesterol associated with primary intracerebral hemorrhage in Bangladeshi population? Bangladesh Critical Care Journal, 6(1), 26-30.
Anwarullah AKM, Habib M, Mohammed QD, Ahmed S, Nahar S. Review of risk factors for stroke: study of 100 cases. Bangladesh J Neurosci 1993;9:11-20.
14. Haque A, Mannan MA. Disease spectrum of neurology outpatient department, IPGMR, Dhaka, during 1995. Bangladesh J Neurosci 1996;2:5-8.
O'donnell, M. J., Xavier, D., Liu, L., Zhang, H., Chin, S. L., Rao-Melacini, P., ... & Yusuf, S. (2010). Risk factors for ischaemic and intracerebral hemorrhagic stroke in 22 countries (the INTERSTROKE study): a case-control study. The Lancet, 376(9735), 112-123.
Tan, A., Gao, Y., Yang, X., Zhang, H., Qin, X., Mo, L., & Mo, Z. (2011). Low serum osteocalcin level is a potential marker for metabolic syndrome: results from a Chinese male population survey. Metabolism, 60(8), 1186-1192.
Jaffre, A., Ruidavets, J. B., Calviere, L., Viguier, A., Ferrieres, J., &Larrue, V. (2014). Risk factor profile by etiological subtype of ischemic stroke in the young. Clinical neurology and neurosurgery, 120, 78-83.