Premature rupture of membrane and perinatal outcome
Abstract
Objective: To find out the complications of a pregnant woman with premature rupture of membrane (PROM) and assess the outcome of it. Materials and
Methods: This prospective study was carried out at the Department of Obstetrics & gynecology of Coronel Malek Medical College Hospital, Manikgonj, Bangladesh from January 2020 to December 2020. All pregnant women admitted with PROM during this period were taken as the study population. After taking proper history they were categorized as a term or preterm PROM on the basis of duration of gestation estimated from 1st day of last menstrual period (LMP), previous antenatal records, clinical examination & also previous ultrasonography (USG) reports. Out of sociodemographic characteristics, age distribution and gravidity were noted. The diagnosis was done on the basis of examination and investigations. All the women with PROM were then followed up, management was given according to protocol and a cesarean section was performed according to indication. Birth weight and Apgar score of newborns were noted after delivery.
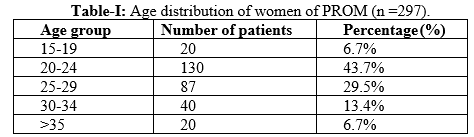
Results: There were 297 cases of PROM recorded among 4461 admitted obstetrical patients over one year period. The hospital incidence of PROM was found to be 6.6%. Among them, 57.6% of patients were admitted at term and 42.4% of patients came before 37 completed weeks of gestation. Most of the pregnant women were between 20-24 years of age (43.7%), 43.2% were primigravida (56.6%) were multigravida. About 48.5% of women presented with different complications associated with PROM. Among which 15.7% of patients had oligohydramnios, 8.5% of patients presented with chorioamnionitis suggested by culture report of the high vaginal swab. Urine for culture and sensitivity was also done. About five (5.2%) developed premature labor before the 37th week of gestation. About 10% of women developed obstetric complications (failed trials) associated with medical diseases. Seventy-seven patients were delivered by cesarean section, 16.2% vaginally, 4.04% patients responded to conservative management and 2.5% patients were referred to a tertiary center for extreme prematurity with associated complicating factors. Most of the babies (38.4%) were born with birth weight between 2.1- 2.5kg and 10.3% of babies were less than 1.5kg.
Conclusion: Term PROM was more in comparison to PPROM and most of them were multigravida. The cesarean section rate was high. Most common complication of was subclinical urogenital infection (53%) next oligohydramnios (25%) & (13.5%) women presented with chorioamnionitis.
Downloads
References
Usha R. Krishna and Monisa H.Shah. Prelabour Rupture of Membranes, Obstetrics and Gynecology for Postgraduates, edited by S.S. Ratnam, K. Bhasker Rao and S. Arulkumaran, 2nd edition-1999; Vol-1, 96-108.
Arias F, Daftary SN, Bhide AG. Premature Rupture of Membrane, Practical Guide to High- Risk Pregnancy & Delivery, A South Asian Perspective, 3rd edition-2008; 240-261.
D.C. Dutta. Prelabour Rupture of the Membranes, Text Book of Obstetrics, 6th edition 2006, 317-320.
Pressman EK, Cavanaugh JL, Woods JR, et al. Physical properties of the chrioamnion throughout gestation. Am J Obstetric Gynecology 2002; 187; 672-5.
Barabas AP. Ehlers-Danlos syndrome associated with prematurity and premature rupture of fetal membranes; possible increase in incidence. Br Med J 1966; 2: 682-4.
McGregor JA. French JL, Lawellin D, et al. Bacterial protease-induced reduction of chorioamnionitis membrane strength and elasticity. Obstet Gynecol 1987; 69: 167-74.
Tasnim S: Clinical Profile and Outcome of Pregnancy in Premature Rupture of Membrane –A Study in Dhaka Medical College Hospital. Dissertation; Bangladesh College of Physicians and Surgeons, 1995.
Begum A; Maternal and Fetal Outcome of Premature Rupture of Membrane –One year Study in Dhaka Medical College Hospital. Dissertation; Bangladesh College of Physicians and Surgeons, 2001.
Begum N; Epidemiology of Premature Rupture of Membrane and Management in Rangpur Medical College Hospital. Dissertation; Bangladesh College of Physicians and Surgeons, 2004.
Bhalerao S, Desai A. Premature rupture of membranes. Jn: Saraiya UB, Rao KB, Chatterjee A, eds. Principles and Practice of Obstetrics& Gynecology (2nd edn). An FOGSI Publication. New Delhi: Jaypee Brothers, 2003: 125.
Daftary SN, Desai SV. Preterm labor and premature rupture of membranes. In: Daftary SN, Desai SV, eds. Selected Topics in Obstetrics & Gynecology (2nd edn). New Delhi: BI Publications, 2006: 128.
Arias F, Tomich PH. Etiology and outcome of low birth weight and preterm infants. Obstetric Gynecology 1982; 60: 277-81.
Romero R, Yoon BH, Mazor M, et al. A comparative study of the diagnostic performance of amniotic fluid glucose, white cell count, interleukin-6 and Gram stain in the detection of microbial invasion in patients with preterm premature rupture of the membranes. Am J Obstetric Gynecology 1993; 169: 839-51.
Johnson J WC, Daikoku NH, Niebyl JR et al. Premature rupture of membranes and prolonged latency. Obstetrics Gynecology 1981; 57: 547-556.
Hein M, Helmig RB, Schonheyder HC, et al. An in vitro study of antibacterial properties of the cervical mucous plug in pregnancy. Am J Obstetric Gynecology 2001; 185.
Mercer BM. Preterm premature rupture of the membranes. Obstetrics Gynecology 2003; 101: 178-93.