Sociodemographic & clinical-pathological evaluation of non-alcoholic fatty liver disease among Bangladeshi population: A single center study
Abstract
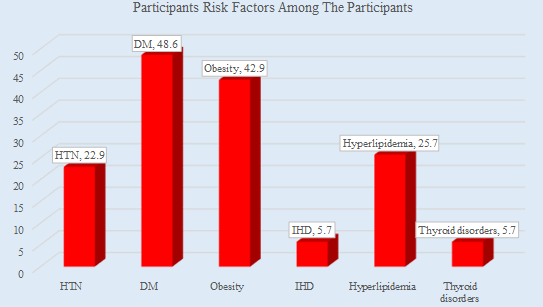
Background: Non-alcoholic fatty liver disease (NAFLD) is a term that refers to a variety of clinicopathological abnormalities in the liver that are a leading cause of hepatic dysfunction and mortality. Obesity, type 2 diabetes, and metabolic syndrome are all contributing to an expanding health problem that goes unreported. There is a scarcity of population-based data in a representative sample of the general population in Bangladesh. Aim of the study: The aims of the study were to evaluate the socio-demographic & clinical-pathological non-alcoholic fatty liver disease among the Bangladeshi population. Method: This cross-sectional study was conducted from July 2019 to December 2019 at Dhaka Medical College Hospital, Bangladesh. This study was purposefully conducted among 35 participants. Results: Among 35 participants, the mean age of the participants was 38.89±8.50 years. Maximum participants (80%) were female and housewives (68.6%). And 60% of participants’ socioeconomic status was a middle-class state. Maximum (48.6%) participants had diabetes mellitus (DM) and obesity (42.9%). The HBs Ag and Anti-HCV were negative among all participants. Their mean body weight was 72.74±8.74 and their mean body height was 61.37±2.67. Here, the odds ratio of the stiffness of liver CAP was 0.75 and the odds ratio of fibroscan of liver CAP was 1.00. Conclusion: NAFLD affects almost one-third of Bangladesh's population. Non-alcoholic fatty liver disease is more common in people with a high BMI (overweight and obese), diabetics, and people in their forties and fifties. The scope of non-alcoholic fatty liver disease is enormous, and healthcare institutions must act quickly. As a result, a focused treatment strategy for non-alcoholic fatty liver disease should be developed.
Downloads
References
Loomba R, Sanyal AJ. The global NAFLD epidemic. Nat Rev Gastroenterol Hepatol. Nature Publishing Group; 2013; 10: 686-690.
Wong RJ, Aguilar M, Cheung R, Perumpail RB, Harrison SA, Younossi ZM, et al. Nonalcoholic steatohepatitis is the second leading etiology of liver disease among adults awaiting liver transplantation in the United States. Gastroenterology. 2015; 148: 547–555. doi: 10.1053/j.gastro.2014.11.039 PMID: 25461851
Rafiq N, Bai C, Fang Y, Srishord M, McCullough A, Gramlich T, et al. Long-term follow-up of patients with nonalcoholic fatty liver. Clin Gastroenterol Hepatol. 2009; 7: 234-238. doi: 10.1016/j.cgh.2008.11. 005 PMID: 19049831
Satapathy SK, Sanyal AJ. Epidemiology and Natural History of Nonalcoholic Fatty Liver Disease. Semin Liver Dis. 2015; 35: 221-235. doi: 10.1055/s-0035-1562943 PMID: 26378640
Duseja A, Chalasani N. Epidemiology and risk factors of nonalcoholic fatty liver disease (NAFLD). Hepatol. Int. 2013; 7: 755-64.
Souza MR, Diniz MD, Medeiros-Filho JE, Araújo MS. Metabolic syndrome and risk factors for non-alcoholic fatty liver disease. Arq. Gastroenterol. 2012; 49: 89-96.
Michelotti GA, Machado MV, Diehl AM. NAFLD, NASH and liver cancer. Nat. Rev. Gastroenterol. Hepatol. 2013; 10: 656-65.
Ray K. NAFLD-the next global epidemic. Nat. Rev. Gastroenterol. Hepatol. 2013; 10: 621
Loomba R, Sanyal AJ. The global NAFLD epidemic. Nat. Rev. Gastroenterol. Hepatol. 2013; 10: 686–90.
Lozano R, Naghavi M, Foreman K et al. Global and regional mortality from 235 causes of death for 20 age groups in 1990 and 2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2013; 380: 2095-128.
Alam S, Mustafa G, Alam M, Ahmad N. Insulin resistance in development and progression of nonalcoholic fatty liver disease. World J. Gastrointest. Pathophysiol. 2016; 7: 211-17.
Rahman S, Ahmed MF, Alam MJ et al. Distribution of liver disease in Bangladesh: a cross-country study. Eurasian J. Hepatogastroenterol. 2014; 4: 25-30.
Hossain MZ, Sikder SS, Zaman K et al. Screening utility, local perceptions, and care-seeking for reported jaundices among respondents lacking signs of icterus in rural Bangladesh. J. Health Popul. Nutr. 2013; 31: 367.
El Khoury AC, Wallace C, Klimack WK, Razavi H. Economic burden of hepatitis C-associated diseases: Europe, Asia Pacific, and the Americas. J. Med. Econ. 2012; 15: 887–96.
Salt WB. Nonalcoholic Fatty Liver Disease (NAFLD): A Comprehensive Review. Insur Med 2004; 36:27-41.
Portillo-Sanchez P et al. High Prevalence of Nonalcoholic Fatty Liver Disease in Patients with Type 2 Diabetes Mellitus and Normal Plasma Aminotransferase Levels. J Clin Endocrinol Metab 2015; 100(6):2231-38.
Lazo M, Clark JM. The Epidemiology of Nonalcoholic Fatty Liver Disease: A Global Perspective: Sociodemographic Differences in the Prevalence of NAFLD. Semin Liver Dis 2008; 28(4):339-350
Harris EH. Elevated Liver Function Tests in Type 2 Diabetes. Clin Diabetes 2005; 23: 115.
Tian, J. et al. Association between bilirubin and risk of Non-Alcoholic Fatty Liver Disease based on a prospective cohort study. Sci Rep 2016; 6: 310-06.
Kwak M, et al. Serum bilirubin levels are inversely associated with nonalcoholic fatty liver disease. Clin Mol Hepatol 2012; 18 (4): 383-90.
Anstee QM, Targher G, Day CP. Progression of NAFLD to diabetes mellitus, cardiovascular disease or cirrhosis. Nat. Rev. Gastroenterol. Hepatol. 2013; 10: 330-44.
Wattacheril J, Sanyal AJ. Lean NAFLD: an underrecognized outlier. Curr. Hepatol. Rep. 2016; 15: 134-9.
Alam S, Noor-E-Alam SM, Chowdhury ZR, Alam M, Kabir J. Nonalcoholic steatohepatitis in nonalcoholic fatty liver disease patients of Bangladesh. World J. Hepatol. 2013; 5: 281-7.
Alam S, Gupta UD, Alam M, Kabir J, Chowdhury ZR, Alam AK. Clinical, anthropometric, biochemical, and histological characteristics of nonobese nonalcoholic fatty liver disease patients of Bangladesh. Indian J. Gastroenterol. 2014; 33: 452-7.