Study of renal profile in children with congenital heart disease in western rural Maharashtra.
Abstract
Introduction: The incidence of congenital heart disease (CHD) is 8-10 per 1000 in India and worldwide and due to recent advancements in diagnostic modalities, early diagnosis and management are possible leading to an increase in long-term survival. Renal involvement is one of the known complications of CHD, especially in cyanotic CHD.
Materials & method: It was a prospective longitudinal study conducted at a tertiary care hospital, including 112 cases ranging from 1 month to 12 years of age with ECHO-proven CHD were studied for the renal profile. Investigations included urea, serum creatinine, serum electrolytes (Na, K, Ca), along with the Urine analysis for protein creatinine ratio. USG abdomen study for kidney size, bladder wall thickness, post-void residue, and pelvi-calceal dilatation was done.
Results: 83.9% of CHD were acyanotic and 16.1% were cyanotic CHD. The most common CHD was VSD (39.3%). Male predominance was noted with Male to Female ratio of 1.24:1.
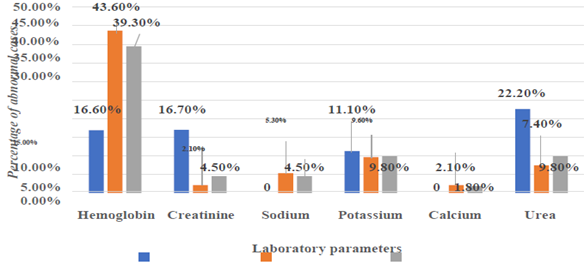
The most common presenting symptom of CHD in our study was poor weight gain (71.4%). Anemia was found in 42 out of the total CHD cases (37.5%). Serum creatinine was raised in 5 patients (4.5%) of CHD. Incidence of elevated creatinine was more common in cyanotic CHD (16.7%) than cyanotic CHD (2.1%) Blood Urea was found to be abnormal in 9.8% of CHD.
Conclusion: Children with CHD are prone to develop renal problems and therefore need monitoring of renal parameters. Serum creatinine levels are most deranged and hence should be checked serially as it is one of the easily available laboratory parameters.
Downloads
References
Puri K, Allen HD, Qureshi AM. Congenital Heart Disease. Pediatrics in Review.2017 Oct;38(10):471–86. https://doi.org/10.1542/pir.2017-0032
Zheng J, Yao Y, Han L, Xiao Y. Renal function and injury in infants and young children with congenital heart disease. Pediatric Nephrology. 2012 Aug 25;28(1):99–104. DOI- 10.1007/s00467-012-2292-8
Dimopoulos K, Diller GP, Koltsida E, Pijuan-Domenech A, Papadopoulou SA, Babu-Narayan SV, Salukhe TV, Piepoli MF, Poole-Wilson PA, Best N, Francis DP, Gatzoulis MA (2008) Prevalence, predictors, and prognostic value of renal dysfunction in adults with congenital heart disease. Circulation 117:2320–2328. doi: 10.1161/CIRCULATIONAHA.107.734921
L. Cordina R, Celermajer DS. Chronic cyanosis and vascular function: implications for patients with cyanotic congenital heart disease. Cardiology in the Young. 2010 Apr 26;20(03):242–53.
Sahai A, Mei C, Schrier RW, Tannen RL. Mechanisms of chronic hypoxia-induced renal cell growth. Kidney International. 1999 Oct;56(4):1277–81.
Vida VL, Mack R, Barnoya J, Larrazabal LA, Lou R, Castañeda AR. The association of renal tubular acidosis and cyanotic congenital heart disease. The Journal of Thoracic and Cardiovascular Surgery. 2005 Nov;130(5):1466–7.
Morgan C, Al-Aklabi M, Garcia Guerra G. Chronic kidney disease in congenital heart disease patients: a narrative review of evidence. Canadian Journal of Kidney Health and Disease [Internet]. 2015 Aug 11 [cited 2021 Feb 24];2. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4531493/
Burlet A, Drukker A, Guignard JP: Renal function in cyanotic congenital heart disease. Nephron 1999; 81:296–300.
Dittrich S, Haas NA, Bührer C, Müller C, Dahnert I, Lange PE: Renal impairment in patients with long-standing cyanotic congenital heart disease. Acta Paediatr 1998; 87:949–954.
Agras PI, Derbent M, Ozcay F, Baskin E, Turkoglu S, Aldemir D, et al. Effect of Congenital Heart Disease on Renal Function in Childhood. Nephron Physiology [Internet]. 2005 [cited 2022 Apr 16];99(1) :p10–5. Available from: https://www.karger.com/Article/Abstract/81797]
El Sayegh S, Ephrem G, Wish JB, Moe S, Lim K. Kidney disease and congenital heart disease: Partnership for life. Frontiers in Physiology. 2022 Aug 19;13.
Vakil RJ. Cardiovascular diseases in India. The American Journal of Cardiology. 1962 Sep;10(3):380–9.
Thakur, J Setal. “Congenital heart disease among school children in Shimlahills.” Indian heart journal vol. 47,3 (1995): 232-5.
Deo B, Jadhav J, Idgampalli N, Deo N, Sabale R. Study of clinical profile of Congenital Heart Disease in pediatric age group. Indian J Basic Appl Med Res. 2015; 4:269-72.
Suresh V, Rao AS, Yavagal ST. Frequency of various congenital heart diseases: analysis of 3790 consecutively catheterized patients. Indian Heart J. 1995 Mar-Apr; 47(2):125-8. PMID: 7590837.
Suguna Bai NS, Vijayalekshmi MS, Nair PM. Congenital malformations of the cardiovascular system. Indian Pediatr. 1988 Sep;25(9):839-44. PMID: 3243633.
Kasturi L, Kulkarni AV, Amin A, Mashankar VA. Congenital heart disease: clinical spectrum. Indian Pediatr. 1999 Sep;36(9):953. PMID: 10744883.
Becker SM, Al Halees Z, Molina C, Paterson RM. Consanguinity and congenital heart disease in Saudi Arabia. Am J Med Genet. 2001 Feb 15;99(1):8-13. Doi: 10.1002/1096-8628(20010215)99:1<8::aid-ajmg1116>3.0.co;2-u. PMID: 11170087.
Gnanalingham MG, Gnanalingham KK, Singh A. Congenital heart disease and parental consanguinity in South India. Acta Paediatr. 1999 Apr;88(4):473-4. doi: 10.1080/08035259950169936. PMID: 10342554.
Emanuel R. Genetics and congenital heart disease. British Heart Journal. 1970 May;32(3):281-291. DOI: 10.1136/hrt.32.3.281. PMID: 4246190; PMCID: PMC487321.
Sanchez-Cascos A. The recurrence risk in congenital heart disease. Eur J Cardiol. 1978 Apr-May;7(2-3):197-210. PMID: 668753.
Amoozgar, Hamid et al. “Undiagnosed Anemia in Pediatric Patients with Congenital Heart Diseases.” International Cardiovascular Research Journal 5 (2011): 70-71.
Lang'o MO, Githanga JN, Yuko-Jowi CA. Prevalence of iron deficiency in children with cyanotic heart disease seen at Kenyatta National Hospital and Mater Hospital Nairobi. East Afr Med J. 2009 Dec;86(12 Suppl): S47-51. doi: 10.4314/eamj.v86i12.62901. PMID: 21591509.
Mukherjee S, Sharma M, Devgan A, Jatana SK. Iron deficiency anemia in children with cyanotic congenital heart disease and effect on cyanotic spells. Med J Armed Forces India. 2018 Jul;74(3):235-240. doi: 10.1016/j.mjafi.2017.07.003. Epub 2017 Aug 18. PMID: 30093766; PMCID: PMC6081276.
Mohamed MS, Rabeea MM, Abu Saif HS, Hammad KS. Assessment of Renal Functions in Infants and Children with Congenital Heart Diseases. The Egyptian Journal of Hospital Medicine. 2019 Jan 1;74(2):219–25.
Ghafari S, Malaki M. Truncus arteriosus: A major cause of proteinuria in children. J Cardiovasc Dis Res. 2011 Oct;2(4):237-40. doi: 10.4103/0975-3583.89809. PMID: 22135483; PMCID: PMC3224445.
Maleki M, Ghaffari S, Ghaffari MR, Samadi M, Rastkar B, Maleki P, Behnam S. Proteinuria in Congenital Heart Disease: Is It a Real Problem? Journal of Cardiovascular and Thoracic Research. 2013 Feb 9;3(1):17-21.