The Efficacy of Serum Procalcitonin as A Reliable Marker for Diagnosis of Neonatal Sepsis
Abstract
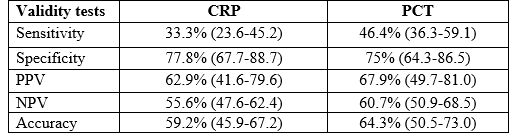
Background: Newborn sepsis (NS) is a major cause of neonatal morbidity and mortality, and it has become a serious global public health issue. Because the clinical appearance of NS can be confounded with non-infectious conditions, the onset of sepsis might be fast, and the clinical process can swiftly subside. Early recognition and diagnosis of neonatal sepsis are difficult because of the variable and non-specific clinical presentation of this condition. Objective: To evaluate the efficacy of serum procalcitonin as a reliable marker in diagnosis of neonatal sepsis. Methods: This cross sectional analytical study was carried out in the Department of Pediatric, Mugda Medical College Hospital, Dhaka, Bangladesh from March to May 2020. Total 55 new-borns with suspected sepsis were included in the study. Specimens of blood were obtained from each neonate prior to commencement of antibiotic for sepsis work up. Serum CRP and procalcitonin levels were measured. Data analysis was performed by using SPSS for windows version 21. Chi-square test, Mann- Whitney U test and Validity test was done to measure the level of significance. Area under the ROC (Receiver operating characteristics) was evaluated. A p value ≤0.05 was considered level of significance. Results: Among total 55 new-borns included in this study, 27(49.09%) new-born were diagnosed as proven sepsis and 28(50.9%) new-born as clinical sepsis. A statistical significant difference was observed between the mean of birth weight in septic and suspected groups. The mean of gestational age (GA) in proved sepsis infants was 31.9 weeks that was lower than two other groups (P< 0.05). The procalcitonin (PCT) was high in 58.2% (500-<2000 pg/ml) new-born and remarkably high (2000-<10000) in 36.4% new-born with sepsis. At a cut-off value > 500pg/ml, the sensitivity of PCT in detecting sepsis was 46.4% its specificity 75%, positive predictive value was 67.9%, and negative predictive value was 60.7% whereas the sensitivity of CRP for predicting sepsis was 33.3%, specificity 77.8%, positive predictive value 62.9% and negative predictive value was 55.6%. The area under the ROC curve for procalcitonin (0.653) was significantly higher than CRP (0.571). Conclusion: In conclusion, the serum levels of PCT is a more reliable marker than the serum levels of CRP or the WBC counts in the early diagnosis of neonatal sepsis and in the evaluation of the response of the disease to the antibiotic therapy. The benefit of measuring serum PCT routinely in the diagnosis and follow-up of neonatal sepsis, is that it reduces the hospital costs.
Downloads
References
Camacho-Gonzalez A, Spearman PW, Stoll BJ: Neonatal infectious diseases: evaluation of neonatal sepsis. Pediatr Clin North Am. 2013, 60:367-89. 10.1016/j.pcl.2012.12.003
Shah BA, Padbury JF: Neonatal sepsis: an old problem with new insights. Virulence. 2014, 5:170-8. 10.4161/viru.26906
Ugarte H, Silva E, Mercan D, De Mendonça A, Vincent JL: Procalcitonin used as a marker of infection in the intensive care unit. Crit Care Med. 1999, 27:498-504. 10.1097/00003246-199903000-00024
Bang AT, Bang RA, Bactule SB, Reddy HM, Deshmukh MD. Effect of home-based neonatal care and management of sepsis on neonatal mortality: field trial in rural India. Lancet 1999; 354:1955-61
Stoll BJ. The global impact of neonatal infection. Clinperinatol 1997; 24:1-21
Gotoff SP. Infection of the neonatal infant. In: Behrman RE; Kliegman RM, Jenson HB, eds. Nelson textbook of pediatrics. 16thed. Philadelphia: WB Saunders Company 2000; 543-49.
Qazi SA, Stoll BJ: Neonatal sepsis: a major global public health challenge. Pediatr Infect Dis J. 2009, 28:S1-2. 10.1097/INF.0b013e31819587a9
National Institute of population Research and Training (NIPORT), Mitra and Associates, and Macro International.2009. Bangladesh Demographic and Health Survey 2007. Dhaka , Bangladesh and Calverton, Maryland USA :National Institute Of Population Research and Training.136
National institute of Population Research and Training, Bangladesh Demographic and Health Survey 1996-1997. Dhaka, National Institute of Population Research and Training,1997.p.252
National Institute of Population Research and Training, Bangladesh Demographic and Health Survey 1999-2000.Dhaka,national Institute of Population Research and Training,2001.p.280
Black S,Kushner I, Samols D. C-reactive protein. Minireview. JBIol Chem 2004;279:48487-48490
Boo NY, Azlina AAN, Rohana J: Usefulness of a semi-quantitative procalcitonin test kit for early diagnosis of neonatal sepsis. Singapore Med J. 2008, 49:204-8.
Bouadma L, Luyt CE, Tubach F, et al.: Use of procalcitonin to reduce patients' exposure to antibiotics in intensive care units (PRORATA trial): a multicentre randomised controlled trial. Lancet. 2010, 375:463-74. 10.1016/S0140-6736(09)61879-1
ACEP Clinical Policies Committee: Clinical policy for children younger than three years presenting to the emergency department with fever. Ann Emerg Med. 2003, 42:530-45. 10.1067/s0196-0644(03)00628-0
Stoll BJ. Infection of the neonatal infant. Kliegman RM, Stanton BF, St. Geme JW III, Schor NF, Behrman RE, editors. Nelson textbook of pediatrics. 19th ed. Philadelphia: Elsevier Saunders, 2011:629–648.
Pierrakos C, Vincent JL. Sepsis biomarker. A review, Critical Care 2010; 14:R 15
Savitri K, Kate A, Gavin B, Edward A. Diagnostic and prognostic biomarkers of sepsis in critical care. J Antimicrob Che mother 2011; 66 Suppl 2:ii33-ii44
Marshall JC, Reinhart K. Biomarkers of Sepsis. Critical care Medicine 2009; 37(7) : 2209-8.
LuytCE, Combes A, Reynoud C, Cottalo G. Diagnostic value of simultaneous measurement of procalcitonin, interleukin-6 and CRP in prediction of Early onset neonatal sepsis. Mediterranean Journals of Hematology and infectious diseases. 2012; 4: 1
Gendrel D, Bohoun C. Procalcitonin as a marker of bacterial infection. Pediatr infect Dis J . 2000; 19 (8):679-87 .
Eberhard Ok. Haubitz M, Brunkhorst FM, Laine S. Usefulness of procalcitonin for differentiation between activity of systemic autoimmune disease and invasive bacterial infection, Arthritis Rheum 1997 ; 40:1250-56
Whicher J, Bienvenu J, Monneret G. Procalcitonin as an acute phase marker. Ann Clin Biochem 2001; 38:483-93.
Lapillonne A, Basson E, Monneret G, Bienvenu J, Salle BL. Lack of specificity of procalcitonin for sepsis diagnosis in premature infants. Lancet 1998;351:1211–1212.
Nylen ES, Jeng J, Jordan MH, Snider RH, Thompson KA, Lewis MS, et al. Late pulmonary sequela following burns: persistence of hyperprocalcitonemia using a 1-57 amino acid N-terminal flanking peptide assay. Respir Med 1995;89:41–46.
Monneret G, Labaune JM, Isaac C, Bienvenu F, Putet G, Bienvenu J. Increased serum procalcitonin levels are not specific to sepsis in neonates. Clin Infect Dis 1998;27:1559–1561.
Cloherty JP, Eichenwald EC, Stark AR. In: Manual of Neonatal care. 6th Ed. Philadelphia : Lippincott Williams and Wilkings; 2008
Naher BS, Mannan MA, Noor K, Shahiddullah M. Role of procalcitonin and C-reactive protein in the diagnosis of neonatal sepsis. Bangladesh Med Res Counc Bull. 2011; 37(2):40-6.
Sucilathangam G, Amuthavallik K, Velvizhi G, Ashiha begum M.A, Jeyamurugan T, Palaniappan N. Early diagnostic markers for neonatal sepsis: Comparing Procalcitonin and C-reactive protein. Journals of Clinical and Diagnostic Research. 2012;6(4): 627-631
Wemberg GA, Powell KR. Laboratory aids for the diagnosis of neonatal sepsis. In infectious disease of the fetus and new-born infant. Eds. Remington JS, Klein JO. Philadelphia, W B Saunders, 5thed 2001:1327-44.
Chiesa C, anero A, Rossi N, Reliability of procalcitonin concentrations for the diagnosis of sepsis in critically ill neonates. Clin Infect Dis.1998; 26(3):664-72.
Monneret G, Labaune JM, Isaac C. Procalcitonin and C-reactive protein level in neonatal infections. Actapaeditr. 1997; 86(2):209-12.
Mohammed I A, Maher Mohammed A W, Louai A S. Procalcitonin as a marker of neonatal of neonatal sepsis in intensive care units. Iran J Med Sci 2010; 35(3): 205-210
Koksal N, Harmanci R, Getinkaya M et al. Role of procalcitonin and CRP in diagnosis and follow up of neonatal sepsis. Turk J Pediatr. 2007; 49:21-9
Kawezymksi P, Piotrowski A. Procalcitonin and C-reactive protein as a marker of neonatal sepsis. Cinekol Pol.2004;75(6):439-44.
Lopez Sastre JB, Perez Solis D, Roques Serradilla V. Evalution of procalcitonin for diagnosis of neonatal sepsis of vertical transmission.BMC Pediatrics 2007; 9.
Hatherill M, TibbySm, Sykes K,Meiser M. Diagnostic markers of infection; comparison of procalcitonin with C-reactive protein and leucocyte count. Arch Dis Child 1999; 81: 417-21.
Sakha K, Husseini M.B, Seyyedsadri N. The role of procalcitonin in the diagnosis of neonatal sepsis and the correlation between procalcitonin and C-reactive protein in these patients. Pak J BiolSci 2008; 11:1785-90.
Boo NY, Nor Azlina AA, Rohana J. Usefulness of a semi-quantitative procalcitonin test kit for the early diagnosis of neonatal sepsis. Singapore Med J 2008; 49:204-08.