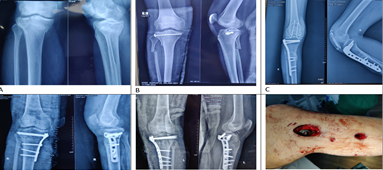
Evaluation and Outcome of Surgical Management of Plateau Fracture- A Study in Shaheed Monsur Ali Medical College, Dhaka, Bangladesh
Abstract
Introduction: Orthopaedic tibial plateau fractures are common. These fractures affect the knee's articular tibia. Plateau fractures may be simple or complicated. Skeletal and ligamentous injuries determine stability.
Methodology: The Department of Orthopaedic and Trauma Surgery at Shaheed Monsur Ali Medical College and Hospital in Dhaka, Bangladesh, performed this prospective study from June to December 2022. This study operated on 22 tibial plateau fracture patients. These individuals have significant injuries from motor vehicle accidents, falls, attacks, etc. These patients were assessed pre- and post-surgery. Schatzker, Hohl-Moore, and AO categorised these examples.
Results: 22 individuals had tibial plateau fractures. Patients averaged 45,4 years old. RTA damaged most patients. Schatzker's classifications called for CRIF, percutaneously cannulated cancellous screws, ORIF with buttress plate with or without bone transplantation, and external fixation for the identified fractures. Post-surgery range of motion started early. Weightless for 6-8 weeks. Weight bearing is delayed until fracture union or 12 weeks. POP casts immobilise unstable fractures for 3-6 weeks. After union, locomotion, weight bearing, and knee range of motion were excellent to very good. Fractures healed as expected. The series showed no non-union. Union averaged 14 weeks (10-22 weeks). Due to the severity of the injuries and infections, ten of the twenty-two surgical cases had excellent outcomes, whereas one had a poor result.
Conclusion: As car accidents grow, so do high-velocity tibial plateau fractures. In depressed and displaced fractures, surgery may stabilise the knee.
Downloads
References
acofsky DJ, Haidukerwych GJ. Tibia plateau fractures. In: Scott WN, editor. Insall & Scott Surgery of the Knee. Philadelphia, PA: Churchill Livingstone; 2006.
Wang SQ, Gao YS, Wang JQ, Zhang CQ, Mei J, Rao ZT. Surgical approach for high-energy posterior tibial plateau fractures. Indian J Orthop 2011; 45:125-31.
Markhardt BK, Gross JM, Monu JU. Schatzker classification of tibial plateau fractures: Use of CT and MR imaging improves assessment. Radiographics 2009; 29:585-97.
Zeltser DW, Leopold SS. Classifications in brief: Schatzker classification of tibial plateau fractures. Clin Orthop Relat Res 2013; 471:371-4.
Wang SQ, Gao YS, 1 Wang JQ, Zhang CQ, Mei J, and Rao ZT. Surgical approach for high-energy posterior tibial plateau fractures. Indian J Orthop. 2011 Mar-Apr; 45(2): 125–31.
Markhardt BK, Gross JM, Monu J. Schatzker Classification of Tibial Plateau Fractures: Use of CT and MR Imaging Improves Assessment. Radio Graphics. March 2009; 29: 585-97.
Zeltser DW, Leopold SS. Classifications in brief: Schatzker classification of tibial plateau fractures. Clin Orthop Relat Res. 2013 Feb; 471(2):371-74.
Mills WJ and Nork SE. Open reduction and internal fixation of High energy tibial plateau fractures. Orthop Clin North Am. 2002; 33: 177-94.
Honkonen SE. Indications for surgical treatment of tibial condyle fractures. Clin Orthop Relat Res. 1994 May; (302):199-205.
Lee JA, Papadakis SA, Moon C and Zalavras CG. Tibial plateau fractures treated with the less invasive stabilisation system. Int Orthop. 2007 June; 31(3): 415–18.
Albuquerque, RP e, Hara R, Prado J, Schiavo L, Giordano V, & Amaral NP do. Epidemiological study on tibial plateau fractures at a level I trauma center. Acta Ortopédica Brasileira. (2013): 21(2), 109-15.
Manidakis N, Dosani A, Dimitriou R, Stengel D, Matthews S, and Giannoudis P. Tibial plateau fractures: functional outcome and incidence of osteoarthritis in 125 cases. Int Orthop. 2010 April; 34(4): 565–70.
Mehin R, O’Brien P, Broekhuyse H, Blachut P, Guy P. Endstage arthritis following tibia plateau fractures: average 10-year follow-up. Can J Surg. 2012 Apr; 55(2):87-94.
Rademakers MV, Kerkhoffs GM, Sierevelt IN, Raaymakers EL, Marti RK. Operative treatment of 109 tibial plateau fractures: five- to 27-year follow-up results. J Orthop Trauma. 2007 Jan; 21(1):5-10.
Gardner MJ, Yacoubian S, Geller D, Suk M, Mintz D, Potter H, et al. The incidence of soft tissue injury in operative tibial plateau fractures: a magnetic resonance imaging analysis of 103 patients. J Orthop Trauma. 2005 Feb; 19(2):79-84.
Schatzker J, McBroom R, Bruce D. The tibial plateau fracture: the Toronto experience 1968-1975. Clin Orthop. 1979; 138:94-104.
Palmer I. Compression fracture of lateral tibial condyle and their treatment. J Bone Joint Surg Am. 1939 Jul 01; 21(3):674-80.
Palmer I. Fractures of the upper end of the tibia. J Bone Joint Surg [Br]. 1951; 33-B: l60-6.
Roberts JM. Fractures of the condyles of the tibia: an anatomical and clinical end-result study of one hundred cases. J Bone Joint Surg [Am]. 1968; 50- A: 1505-2l.
Pasa L, Kelbl M, Suchomel R, Procházka V, Filipínský J.Treatment of intra- articular proximal tibial evaluation of two- to seven-year follow-up. Acta Chir Orthop Traumatol Cech. 2007 Oct; 74(5):336-41.
Urruela AM, Davidovitch R, Karia R, Khurana S, Egol KA. Results following operative treatment of tibial plateau fractures. J Knee Surg. 2013 Jun; 26(3):161-5.